
by Comprehensive Orthopaedics | Jan 10, 2023 | Elbow, pain, Wellness
Bicep tears are common, but many people fail to realize that the pain they’re feeling is actually caused by their bicep, not their shoulder. You may not realize it, but you put a lot of strain on your shoulders when lifting weights or playing common sports like...

by Comprehensive Orthopaedics | Dec 13, 2022 | Anti-aging, arthritis, Wellness
Olympic athletes aren’t like the rest of the population — but this time it’s in a far less positive way. Two new studies show that athletes who performed at the top of their sport have a higher risk of developing arthritis and joint pain in later...

by Comprehensive Orthopaedics | Nov 15, 2022 | Wellness
Adult cancer survivors, particularly those who have undergone chemotherapy, have an increased risk for serious pelvic and vertebral fractures, new research shows. “These findings are important as the number of cancer survivors living in the United States is...
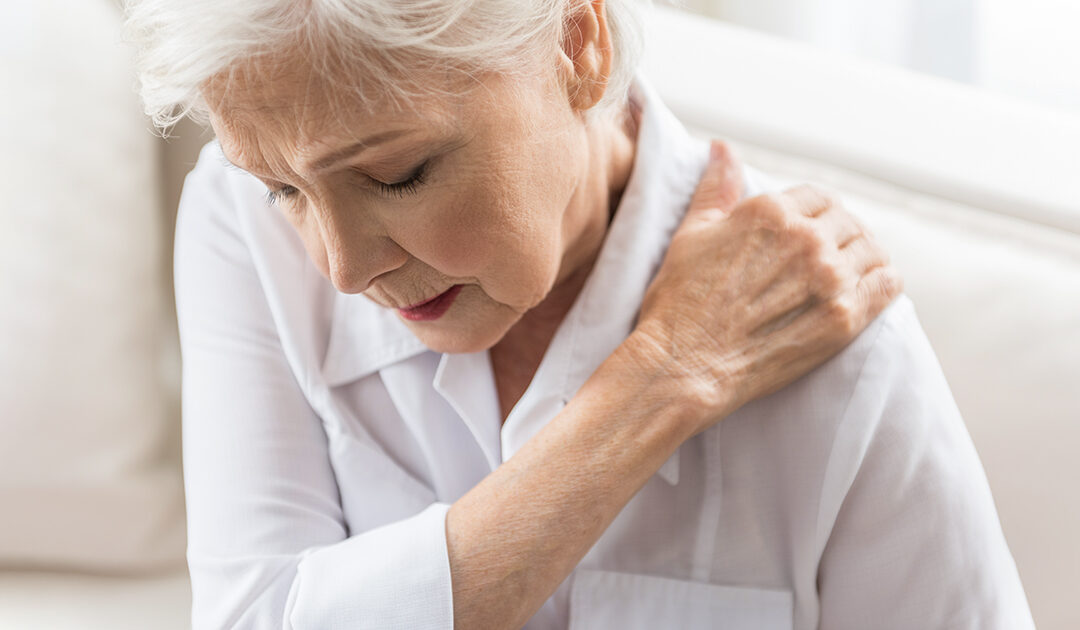
by Comprehensive Orthopaedics | Oct 19, 2022 | Shoulder, Wellness
Arthritis is a frequently overlooked cause of shoulder pain. Find out how you can determine if your shoulder pain is actually being caused by arthritis. An aching shoulder is a common orthopedic complaint. But how do you know if the pain is caused by arthritis or...

by Comprehensive Orthopaedics | Sep 15, 2022 | Anti-aging, arthritis, Wellness
Aching joints are common for people over 50, but it’s still important to talk to a doctor about it rather than endlessly self-medicating, experts say. Now, a new poll from the University of Michigan breaks down joint pain, its impact on those who responded to the...

by Comprehensive Orthopaedics | Sep 8, 2022 | Ankle, Wellness
A sprained ankle can be painful and debilitating, but luckily your recovery time will usually be short — especially if you take steps to protect your ankle as it heals! Joint sprains are a remarkably common part of life for both athletes and non-athletes alike. With...






