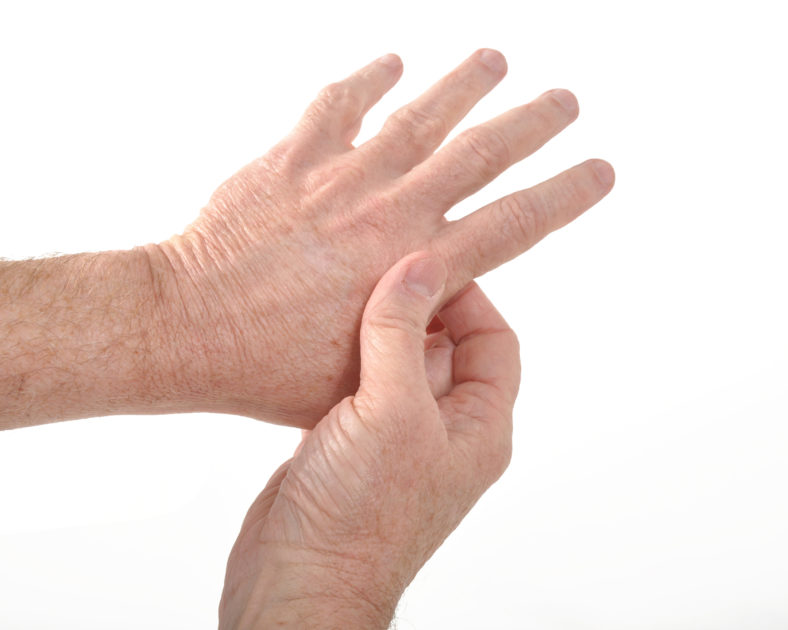
by Comprehensive Orthopaedics | May 22, 2019 | Anti-aging, arthritis, Hand, pain, Wellness
FRIDAY, May 10, 2019 (HealthDay News) — Difficulties with daily activities such as dressing, walking and eating can be seen in rheumatoid arthritis patients a year or two before they’re diagnosed, a new study shows. “This is a new finding, and a...

by Comprehensive Orthopaedics | Apr 25, 2019 | anatomy, Ankle, Anti-aging, Elbow, Foot, Hand, Hip, Knee
(HealthDay News) — Most people have popping and cracking of their joints, especially as they age. Though the reasons behind these sounds are unclear, doctors think they may be caused by ligaments stretching and releasing, or the compression of nitrogen bubbles....

by Comprehensive Orthopaedics | Mar 19, 2019 | Hand, pain, Wellness, Wrist
FRIDAY, March 1, 2019 (HealthDay News) — You use your hands nearly every minute of the day, so any time they hurt it’s important to find out why. Certain conditions can affect people who do the same hand movements for hours every day. Repetitive strain...

by Comprehensive Orthopaedics | Mar 5, 2019 | arthritis, Hand, Wellness
FRIDAY, March 1, 2019 (HealthDay News) — You use your hands nearly every minute of the day, so any time they hurt it’s important to find out why. Certain conditions can affect people who do the same hand movements for hours every day. Repetitive strain...

by Comprehensive Orthopaedics | Mar 4, 2019 | Anti-aging, Hand, pain, Wellness, Wrist
(HealthDay News) — Carpal tunnel syndrome (CTS) occurs when pressure is placed on a nerve stretching from the arm to the hand. Often, this is due to stress on the hands and wrists. Adjusting your daily routine can help prevent CTS. NYU Langone Health offers...

by Comprehensive Orthopaedics | Nov 15, 2018 | Hand, Wellness
Carpal tunnel syndrome occurs when the nerve that runs from the forearm to the wrist becomes squeezed or compressed. The condition can be caused by an injury to the wrist, stress to the joint, rheumatoid arthritis, or repetitive motion of the hand and wrist. Here are...






