Hip Replacement surgery
Hip Replacement Surgeons in Kenosha and Burlington, WI
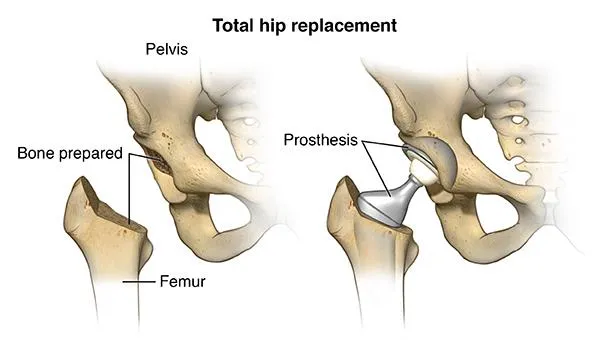
What is hip replacement surgery?
Hip replacement, also called total hip arthroplasty, is a surgical procedure to replace a worn out or damaged hip joint with a prosthesis (an artificial joint). This surgery may be an option after a hip fracture or for severe pain due to arthritis.
Various types of arthritis may affect the hip joint:
- Osteoarthritis. This is a degenerative joint disease that affects mostly middle-aged and older adults. It may cause the breakdown of joint cartilage and adjacent bone in the hips.
- Rheumatoid arthritis. This type of arthritis causes inflammation of the synovial lining of the joint and results in excessive synovial fluid. It may lead to severe pain and stiffness.
- Traumatic arthritis. This is arthritis resulting from an injury. It may also cause damage to the hip cartilage.
The goal of hip replacement surgery is to replace the parts of the hip joint that have been damaged and to relieve hip pain that can’t be controlled by other treatments.
A traditional hip replacement involves an incision several inches long over the hip joint. A newer approach that uses one or two smaller incisions to perform the procedure is called minimally invasive hip replacement. However, the minimally invasive procedure is not suited for all people who need hip replacement. Your doctor will determine the best procedure for you.
Why might I need hip replacement surgery?
What are the risks of hip replacement surgery?
How do I get ready for hip replacement surgery?
What happens during hip replacement surgery?
What happens after hip replacement surgery?
Hip replacement surgery is a treatment for pain and disability in the hip. The most common condition that results in the need for hip replacement surgery is osteoarthritis.
Osteoarthritis causes loss of joint cartilage in the hip. Damage to the cartilage and bones limits movement and may cause pain. People with severe pain due to degenerative joint disease may be unable to do normal activities that involve bending at the hip, such as walking or sitting, because they are painful.
Other forms of arthritis, such as rheumatoid arthritis and arthritis that results from a hip injury, can also lead to degeneration of the hip joint.
Hip replacement may also be used as a method of treating certain hip fractures. A fracture is an injury often from a fall. Pain from a fracture is severe and walking or even moving the leg is difficult.
If medical treatments are not effectively controlling arthritis pain, hip replacement may be an option. Some medical treatments for degenerative joint disease may include:
- Anti-inflammatory medications
- Glucosamine and chondroitin sulfate
- Pain medications
- Limiting painful activities
- Assistive devices for walking (such as a cane)
- Physical therapy
There may be other reasons for your healthcare provider to recommend a hip replacement surgery.
As with any surgical procedure, complications can occur. Some possible complications may include:
- Bleeding
- Infection
- Blood clots in the legs or lungs
- Dislocation
- Need for revision or additional hip surgery
- Nerve injury resulting in weakness or numbness
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your healthcare provider prior to the procedure.
- Your healthcare provider will explain the procedure to you and offer you the chance to ask any questions that you might have about the procedure.
- You may be asked to sign a consent form that gives your permission to do the procedure. Read the form carefully and ask questions if something is not clear.
- In addition to a complete medical history, your healthcare provider may perform a complete physical exam to ensure you are in good health before undergoing the procedure. You may undergo blood tests or other diagnostic tests.
- Tell your healthcare provider if you are sensitive to or are allergic to any medications, latex, tape, and anesthetic agents (local and general).
- Tell your healthcare provider of all medications (prescribed and over-the-counter) and herbal supplements that you are taking.
- Tell your healthcare provider if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medications, aspirin, or other medications that affect blood clotting. It may be necessary for you to stop these medications prior to the procedure.
- If you are pregnant or suspect that you are pregnant, you should notify your healthcare provider.
- You will be asked to fast for 8 hours before the procedure, generally after midnight.
- You may receive a sedative prior to the procedure to help you relax.
- You may meet with a physical therapist prior to your surgery to discuss rehabilitation.
- Stop smoking, as smoking can delay wound healing and slow down the recovery period.
- Lose weight if needed.
- Perform conditioning exercises as prescribed to strengthen muscles.
- Arrange for someone to help around the house for a week or two after you are discharged from the hospital.
- Based on your medical condition, your healthcare provider may request other specific tests or exams.
Hip replacement requires a stay in a hospital. Procedures may vary depending on your condition and your doctor’s practices.
Hip replacement surgery is performed while you are asleep under general anesthesia or sedated under spinal anesthesia. Your anesthesiologist will discuss this with you in advance.
Generally, hip replacement surgery follows this process:
- You will be asked to remove clothing and will be given a gown to wear.
- An intravenous (IV) line may be started in your arm or hand.
- You will be positioned on the operating table.
- A urinary catheter may be inserted (after you are asleep).
- The anesthesiologist will continuously monitor your heart rate, blood pressure, breathing, and blood oxygen level during the surgery.
- The skin over the surgical site will be cleansed with an antiseptic solution.
- The doctor will make an incision in the hip area.
- The doctor will remove the damaged parts of the hip joint and replace them with the prosthesis. The hip prosthesis is made up of a stem that goes into the femur (thighbone), the ball (head joint) that fits into the stem, and a cup that is inserted into the socket of the hip joint. The stem and cup are made of metal. The ball may be made of metal or ceramic. The cup has a liner that may be made of plastic or ceramic. The two most common types of artificial hip prostheses used are cemented prostheses and uncemented prostheses. A cemented prosthesis attaches to the bone with surgical cement. An uncemented prosthesis attaches to the bone with a porous surface onto which the bone grows to attach to the prosthesis. Sometimes, a combination of the two types is used to replace a hip.
- The incision will be closed with stitches or surgical staples.
- A drain may be placed in the incision site to remove fluid.
- A sterile bandage or dressing will be applied.
In the hospital
After the surgery you will be taken to the recovery room for observation. Once your blood pressure, pulse, and breathing are stable and you are alert, you will be taken to your hospital room. Hip replacement surgery usually requires you to stay in the hospital for several days.
It is important to begin moving the new joint after surgery. A physical therapist will meet with you soon after your surgery and plan an exercise rehabilitation program for you. Your pain will be controlled with medication so that you can participate in the exercise. You will be given an exercise plan to follow both in the hospital and after discharge.
You will be discharged home or to a rehabilitation center. In either case, your healthcare provider will arrange for continuation of physical therapy until you regain muscle strength and good range of motion.
At home
Once you are home, it is important to keep the surgical area clean and dry. Your healthcare provider will give you specific bathing instructions. The stitches or surgical staples will be removed during a follow-up office visit.
Take a pain reliever for soreness as recommended by your healthcare provider. Aspirin or certain other pain medications may increase the chance of bleeding. Be sure to take only recommended medications.
Notify your healthcare provider to report any of the following:
- Fever
- Redness, swelling, bleeding, or other drainage from the incision site
- Increased pain around the incision site
- Numbness and/or tingling in the affected leg
You may resume your normal diet unless your healthcare provider advises you differently.
You should not drive until your healthcare provider tells you to. Other activity restrictions may apply. Full recovery from the surgery may take several months.
It is important that you avoid falls after your hip replacement surgery because a fall can result in damage to the new joint. Your therapist may recommend an assistive device (cane or walker) to help you walk until your strength and balance improve.
Making certain modifications to your home may help you during your recovery. These modifications include, but are not limited to, the following:
- Proper handrails along all stairs
- Safety handrails in the shower or bath
- Shower bench or chair
- Raised toilet seat
- Stable chair with firm seat cushion and firm back with two arms, which will allow your knees to be positioned lower than your hips
- Long-handled sponge and shower hose
- Dressing stick
- Sock aid
- Long-handled shoe horn
- Reaching stick to grab objects
- Firm pillows to raise the hips above the knees when sitting
- Removing loose carpets and electrical cords that may cause you to trip
Your healthcare provider may give you additional or alternate instructions after the procedure, depending on your particular situation.

Next steps
Before you agree to the test or the procedure make sure you know:
-
The name of the test or procedure
-
The reason you are having the test or procedure
-
The risks and benefits of the test or procedure
-
When and where you are to have the test or procedure
-
When and how will you get the results
-
How much will you have to pay for the test or procedure

