
by Comprehensive Orthopaedics | Oct 30, 2017 | Hip, pain, Pelvis, surgery, Wellness
Icy winter weather may lead to fewer hip fractures than many believe. Most fall-related hip fractures among elderly people in a New England study occurred in warm months and indoors — with throw rugs a common culprit. “Given the results of this study, it...

by Comprehensive Orthopaedics | Oct 25, 2017 | Knee, surgery
Athletes in high impact sports or sports that require a lot of running and jumping are prone to knee injuries. kneecap dislocations most often happen as a result of trauma, such as when a football player is tackled, or a soccer players falls hard on his knees. The...
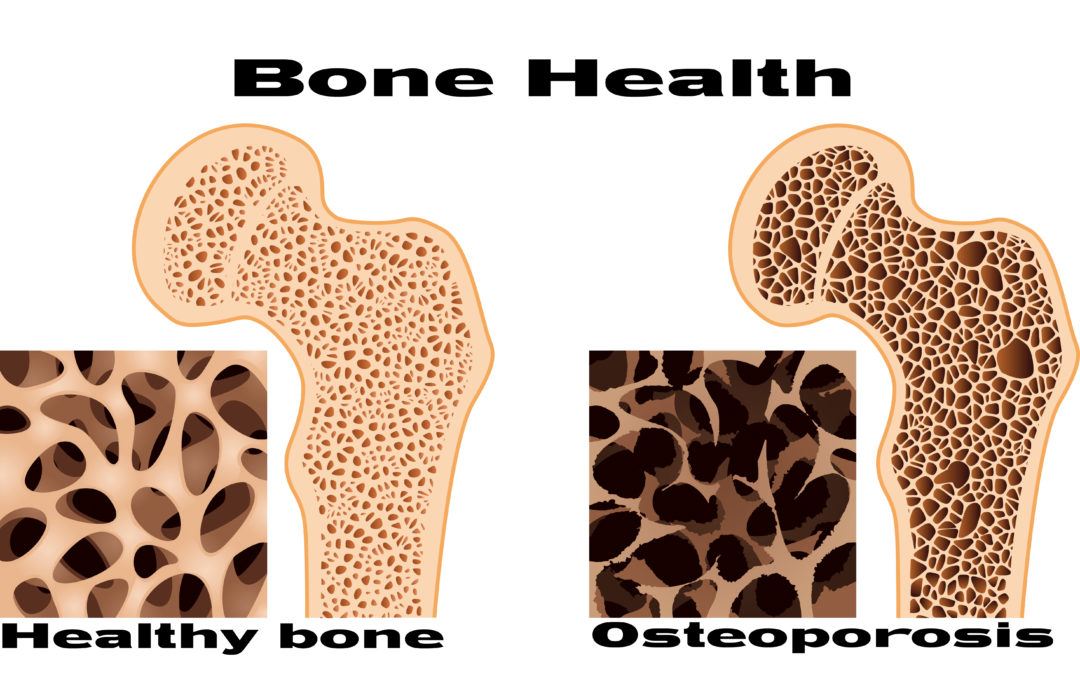
by Comprehensive Orthopaedics | Oct 9, 2017 | Anti-aging, Wellness
Bone health is literally something you build on throughout your life, not just as a child. And the efforts you put in now will keep bones strong and help prevent the bone-thinning disease osteoporosis later on, as you age. Most of the 10 million Americans living with...

by Comprehensive Orthopaedics | Oct 2, 2017 | Anti-aging, Wellness
The link between exercise and good health is a strong one. Still, many people — particularly older adults — find it difficult to take part in formal exercises, and become less physically active over time. But scientists are discovering that if you keep...




